Feb 2, 2022PA Surgeon Pioneers Faster Recovering ACL Surgery
When a budding girls high school basketball player in Pennslyvania saw her season cut short due to a torn ACL during summer league play, Cayleigh Walker and her family turned to one of the best.
Dr. Matthew A. Varacallo is the medical director of Orthopedic Robotic Surgery at Penn Highlands Healthcare — a top 65 knee replacement surgeon according to Beckers’ ACS Review.
 Along with Dr. Chad Lavender, Varacallo pioneered the fertilized ACL technique. Currently, they are the only two surgeons in the country using this technique.
Along with Dr. Chad Lavender, Varacallo pioneered the fertilized ACL technique. Currently, they are the only two surgeons in the country using this technique.
Below is a story from The Courier Express about Varacallo’s pioneering technique.
“Typically, when an ACL tear occurs, one-third of the athletes re-tear the same side or injure the other knee; but, the theory behind the fertilized ACL technique is to improve and expedite bone tunnel healing rates, followed by graft revascularization and ligamentization (the process by which the tendon becomes a ligament) to improve graft function and incorporation into the knee joint,” explained Dr. Varacallo.
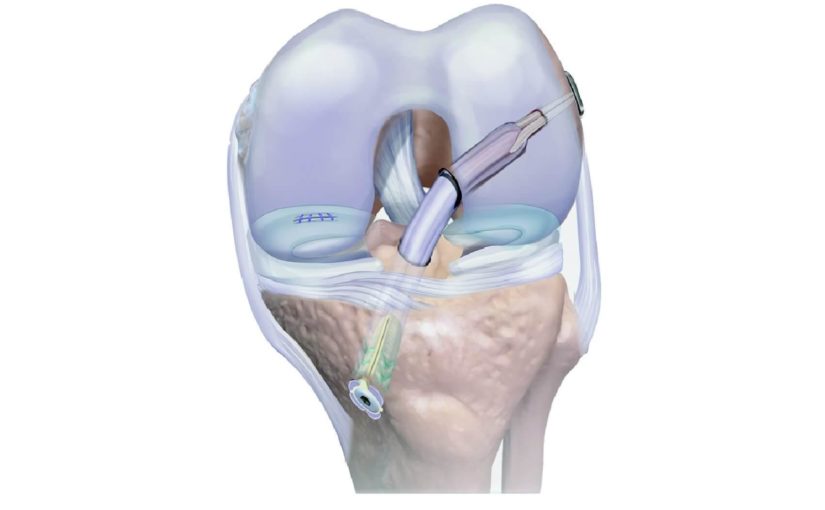
The fertilized ACL procedure begins when bone marrow is removed from the tibia — the long bone on the inside of the lower leg — which is rich in growth hormone and stem cells. A specialized perfusionist takes 60 milliliters of the bone marrow and spins it down to bone marrow aspiration concentrate (BMAC) which is used to initiate healing. The BMAC is mixed with bone graft. Small tunnels are then made in the femur and tibia to place the graft during the procedure. The bone graft mixture and stem cells/growth factors are then injected into the tunnels to help stimulate them to heal faster. Once the tunnels heal, the tendon can in theory possibly transform into a ligament faster.
 “This is truly a cutting-edge procedure,” explained Dr. Varacallo. “In traditional ACL surgeries, the pressurized tunnels can be risk factors for re-injury because they can take up to six or seven months to heal. However, with the fertilized ACL procedure, the tunnels heal faster because the graft starts to incorporate into the body faster. In fact, four weeks post-surgery, you cannot even see the bone tunnels,” the surgeon added.
“This is truly a cutting-edge procedure,” explained Dr. Varacallo. “In traditional ACL surgeries, the pressurized tunnels can be risk factors for re-injury because they can take up to six or seven months to heal. However, with the fertilized ACL procedure, the tunnels heal faster because the graft starts to incorporate into the body faster. In fact, four weeks post-surgery, you cannot even see the bone tunnels,” the surgeon added.
» ALSO SEE: When is the most effective time to exercise?
Dr. Varacallo considers Cayleigh the poster child for successful ACL reconstruction because she is achieving milestones sooner than expected, and Samantha (Sam) Morgan, MS ATC PES, a certified athletic trainer with Penn Highlands Healthcare as well as with the Clearfield Area School District agrees.
“Three days following surgery, Cayleigh began rehab, and at three and one half weeks post-op she was running, and six to seven weeks following surgery she was punting a soccer ball. In contrast, with traditional ACL surgery, we would not see that type of progress until three or four months post-op,” Ms. Morgan detailed.


