Aug 7, 2021The Physical Exam of the Concussed Athlete
Sports are second only to motor vehicle crashes as the leading cause of traumatic brain injury among people aged 15 to 24. Concussions in high school athletics represent 8.9% of all injuries occurring from sports. It has been reported that football and soccer have the highest rates of concussion in high school athletics. The athletic trainer’s evaluation is a critical component to the management of the post-concussion athlete from the time the injury occurs to when the athlete returns to the field of play.
Athletic trainers are excellent at recognizing when an athlete potentially has a concussion on the sidelines during a sporting event by performing the SCAT5 which is the standard of care for helping diagnose an athlete with a sports-related concussion. However, SCAT5 is not enough. The athletic trainer, working in conjunction with the team physician, needs a comprehensive plan for the on-the-field examination and the follow-up examination of the post-concussed athlete. This plan will, in turn, help the athlete’s medical team determine the appropriate rehabilitation prior to starting the return to play process. Athletic trainers are at the forefront with respect to concussions and the management of concussed athletes. However, even athletic trainers will benefit from reviewing traditional approaches and new information on the important elements of the multidimensional approach to the clinical physical exam.
 This paper is a guide for the athletic trainer when managing a concussed athlete to ensure that the appropriate rehabilitation techniques are used for each individual athlete. I have had the opportunity to work and observe Dr. Robert Franks, who is a board-certified family practice physician with a certificate of added qualification in Sports Medicine at Rothman Orthopaedic Institute, he specializes in medical orthopedics, sports medicine, and is one of the nation’s leaders in sports-related concussion management. My work with and observations of Dr. Robert Franks with post-concussed athletes has led to the development of a comprehensive clinical evaluation of the post-concussion athlete to monitor recovery, along with the development of appropriate concussion therapy.
This paper is a guide for the athletic trainer when managing a concussed athlete to ensure that the appropriate rehabilitation techniques are used for each individual athlete. I have had the opportunity to work and observe Dr. Robert Franks, who is a board-certified family practice physician with a certificate of added qualification in Sports Medicine at Rothman Orthopaedic Institute, he specializes in medical orthopedics, sports medicine, and is one of the nation’s leaders in sports-related concussion management. My work with and observations of Dr. Robert Franks with post-concussed athletes has led to the development of a comprehensive clinical evaluation of the post-concussion athlete to monitor recovery, along with the development of appropriate concussion therapy.
Athletes who have sustained a concussion can experience any or all of approximately 21 different symptoms, including a headache, dizziness, confusion, and difficulty concentrating as well as cognitive, vestibular, and ocular motor impairments. Most researchers and clinicians can agree that on average sports-related concussion symptoms resolve within about 7-10 days post-injury. Researchers have identified several post-injury factors that may negatively affect a patient’s recovery. The occurrence of post-traumatic migraine symptoms following concussion (headache with nausea and photo- and/or phonosensitivity), immediate dizziness, and sub-acute (within 3–7 days) fogginess, difficulty concentrating, vomiting, dizziness, nausea, headache, slowness, imbalance, photo/phonosensitivity, and numbness predict longer than normal (i.e. 14–21 days) recovery times.
Researchers have reported that vestibular impairments are common following a sports-related concussion and approximately 50% of athletes report dizziness within the first few days post-concussion. Ocular-motor problems are experienced by approximately 1/3 of athletes in the first week following a concussion. It is likely that vestibular and ocular-motor symptoms may impair an adolescent athlete’s ability to learn and participate in athletics because symptoms include dizziness, headache, vertigo, fogginess, motion sensitivity, disequilibrium, postural or gait imbalance, gaze instability, blurred vision, or diplopia. Vision symptoms can include abnormal eye movements and visual instability. Vestibular and ocular-motor symptoms affect the learning of adolescents by making it difficult for the student-athlete to read, copy notes, paying attention to visual tasks, standing quickly, or walking in a crowded environment of the school can be a challenge, and the student-athlete might have problems with aspects of a typical day of school (slide presentations, movies, smartboards, computers, handheld computers (tablets and cell phones), and artificial lighting). The vestibular ocular-motor symptoms can affect the student-athletes ability to run, balance, sports-specific movements, and the inability to perform physical exertion. The detailed physical exam of an athlete with a concussion can reveal which vestibular ocular motor symptoms that the athlete is currently experiencing which then can help the athletic trainer choose the appropriate rehabilitation.
Currently, clinicians have no “stand-alone” objective tool to diagnose or treat sports-related concussions. Symptoms score and neurocognitive testing have shown promise for predicting an athlete’s recovery and time until return to play. The use of vestibular ocular-motor screening (VOMS) allows clinicians to better identify patients who may require specialized vestibular and vision therapy early in the recovery process. This better understanding of vestibular ocular-motor symptoms and their relationship to recovery can better help the athletic trainer develop rehabilitation and ultimately help improve outcomes for their patients in the quest to return to full learning and athletic participation. Athletic trainers and the concussion management team must use a multidimensional approach to assess and manage sports-related concussions since we currently do not have a “stand-alone” objective tool to diagnose sports-related concussions or a way to determine the length of recovery.
 The athletic trainer should use all the resources and tools they have at their disposal to help with the assessment and treatment of the concussed patient. Any athlete who is exhibiting the signs or symptoms of a sports-related concussion or another head injury during practice or competition must be immediately removed from play and activities and may not return to the practice or competition that day. In the event that the athlete has signs and symptoms of a concussion and the athletic trainer should perform the examination on the sidelines or within the athletic training facility, whichever is deemed appropriate by the medical staff at the time of injury.
The athletic trainer should use all the resources and tools they have at their disposal to help with the assessment and treatment of the concussed patient. Any athlete who is exhibiting the signs or symptoms of a sports-related concussion or another head injury during practice or competition must be immediately removed from play and activities and may not return to the practice or competition that day. In the event that the athlete has signs and symptoms of a concussion and the athletic trainer should perform the examination on the sidelines or within the athletic training facility, whichever is deemed appropriate by the medical staff at the time of injury.
The athletic trainer should perform the physical examination of the athlete periodically during the recovery phase of the injured athlete to assess the athlete’s road to recovery and to determine what adjustments need to be made to the rehabilitation plan. The multidimensional post-concussion evaluation should be conducted at a minimum weekly on the athletic and should take the athletic trainer about 15 to 20 minutes to perform. The evaluation should consist of assessment tools but not limited to which include a detailed history of the event, symptom score, SCAT5, balance testing, and Vestibular Ocular-Motor Screen (VOMS). All findings of the concussion assessment should be made available to the athlete’s medical team to ensure all parties are on the same page and all efforts are coordinated for the best interest of the athlete.
» ALSO SEE: Information on Inflammation
The detailed history of the event and athlete’s medical history is a critical component in the assessment process which should include:
- How many head injuries has the patient had in the past?
- When did they occur?
- How did they occur?
- What type of symptoms did the athlete have?
- How long did the symptoms last?
- Did they lose consciousness?
- Did they have amnesia (anterograde or retrograde)?
- Are the current symptoms and injury associated with loss of consciousness or amnesia and what type?
- Does the athlete have a history of motion sickness?
- What kind of headache does the athlete have and does it worsen with exertion or mental work?
- Does the athlete get dizzy with movement?
- Is the athlete more sensitive to light or noise?
- Is the athlete more distracted?
- Is the athlete moody or irritable?
- Does the athlete feel “foggy” or “removed”?
- How long did it take the athlete to recover from past concussions?
- Did the athlete have incidents/symptoms from any hits to the chest, neck, or face that radiated to the head (e.g., whiplash) that were not reported as a concussion?
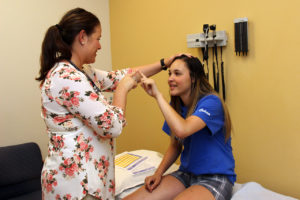 The physical examination should first include the SCAT5 and the BESS examination, which should be conducted on the sidelines but when appropriate the physical exam should be conducted in a distraction-free environment (e.g., locker room or medical room) rather than on the sideline. The SCAT5 alone should take about 10 minutes to thoroughly conduct. Additionally the SCAT5 this a physical exam that consists of vital signs, analyses of speech and gait, cranial nerve testing, visual field testing, upper extremity sensation, lower extremity sensation, range of motion, muscle strength, deep tendon reflexes, Romberg’s test, pronator drift test, tandem walk, heel to shin test, finger to nose testing, and vestibular ocular-motor screening (VOMS). It is highly recommended that the athletic trainer and medical staff include VOMS testing as part of the physical exam because of the importance the vestibular-ocular system plays in concussions.
The physical examination should first include the SCAT5 and the BESS examination, which should be conducted on the sidelines but when appropriate the physical exam should be conducted in a distraction-free environment (e.g., locker room or medical room) rather than on the sideline. The SCAT5 alone should take about 10 minutes to thoroughly conduct. Additionally the SCAT5 this a physical exam that consists of vital signs, analyses of speech and gait, cranial nerve testing, visual field testing, upper extremity sensation, lower extremity sensation, range of motion, muscle strength, deep tendon reflexes, Romberg’s test, pronator drift test, tandem walk, heel to shin test, finger to nose testing, and vestibular ocular-motor screening (VOMS). It is highly recommended that the athletic trainer and medical staff include VOMS testing as part of the physical exam because of the importance the vestibular-ocular system plays in concussions.
Let’s take a closer look at some of these important physical exam tests that should be performed on the post-concussion patient in the clinic:
Romberg’s Test: (Balance/ Proprioception Testing)
The athlete is asked to stand with his or her feet close together, arms by the side, and eyes open. Any significant swaying or tendency to fall is noted. The athlete is then asked to close his or her eyes. Postural swaying is again noted and compared with that observed with open eyes.
Pronator Drift Test: (Proprioception Testing)
The athlete is asked to hold his or her arms outstretched with palms facing upward. The athlete is then asked to close his or her eyes. At this point, the athlete must rely on proprioception alone to maintain the position of the arms. If the arm drifts downward and the palms turn towards the floor the supinator muscles in the upper arm are weaker than the pronator muscles which might indicate an upper motor neuron lesion.
Tandem Walk: (Coordination Testing)
The athlete walks in a forward direction as quickly and as accurately as possible along with an alternate foot heel-to-toe gait ensuring that the athlete is adjoining their heel and toe on every step. Athletes should complete the test in 14 seconds. This test is best performed without shoes on. Failure of the exam is indicated if the athlete steps off the line, have a separation between their heel and toe, or if the athlete touches or grabs the examiner or an object.
Heel to Shin Test: (Coordination Testing)
The athlete slides the heel of their foot down the shin (the shoe should be removed). The athlete repeats the movement with the other foot. An abnormal exam is when the athlete is unable to perform the movement rapidly.
Finger to Nose Testing: (Coordination Testing)
This test is performed by the athlete fully extending their arm and touching the athletic trainer’s finger. Then touching the nose repeats the motion from extending an arm to the nose. To increase the difficulty the athletic trainer can move their finger in different locations. An abnormal exam is when the athlete cannot perform the task smoothly and rapidly.
VOMS: (Vestibular-Ocular Motor Screening) Modified from Mucha A, Collins MW, Elbin RJ, Furman JM, Troutman‐Enseki C, DeWolf RM, Marchetti G, Kontos AP.
Smooth Pursuits – The capacity for the athlete to follow a slowly moving target.
Saccades – The capacity for the athlete’s eyes to moving quickly between two targets.
Convergence – The capacity for the athlete to view a near target without double vision.
Vestibular-Ocular Reflex (VOR) Test – The capacity for the athlete to stabilize vision as the head moves.
Visual Motion Sensitivity (VMS) Test – The athlete’s capacity to inhibit vestibular-induced eye movements using vision.
Brief Instructions: patient seated unless noted otherwise. 9‐40 y/o, 1 day or > after injury
Pursuit ‐ One stick, 3′ away and level with athlete’s nose, move stick slowly 1.5′ to the left and 1.5′ to the right. Repeat moving stick vertically. Slow: 2 seconds to go L to R & again L to R. 2 repetitions each direction.
Saccade ‐ Start 2 sticks, 3 feet away and level with athlete’s nose. Each stick 1.5′ to the left and right of the nose. Look over & back 10x. Repeat vertically. The athlete is to move eyes as fast as they can.
NPC ‐ One stick, 3′ away and level with patient’s nose. Move stick slowly towards the nose. Stop when they report seeing double or you see an eye turn/drift. Measure distance to the nose.
VOR ‐ Hold one stick, 3′ away and level with the athlete’s nose. The speed of head movement, 180 bpm. The patient turns their head 20 degrees left and right, 10 times maintaining focus on the target. Repeat vertically.
Visual Motion Sensitivity ‐ Standing, the patient holds a stick or thumb; arms reach in front of the nose. While maintaining fixation on a stick, rotate head arms and trunk left and right 80 degrees 5x at 50 bpm.
Once the detailed history and physical assessment of the concussed athlete have been concluded the athlete might need to be referred to a physician trained in the evaluation and treatment of sports-related concussions depending on your state’s concussion laws. If the athlete has unresolved symptoms of a concussion longer than the typical recovery time of seven to ten days, it is recommended that the athletic trainer refer the patient to a physician trained in the management of a concussion. Again, all findings from the physical examination should be given to the attending physician, along with any neurocognitive testing results including baseline results if available.
It is imperative that we understand that the SCAT5 exam alone is not enough when examining the student-athlete who has sustained a sports-related concussion. The athletic trainer needs to perform a detailed examination that includes all the above tests and assessments so that there is a thorough blueprint for the athlete’s medical team. The post-concussion physical exam will be critical in the development of the appropriate treatment plan, return to learn plan, and the return to play protocol. The detailed examination performed by the athletic trainer at the time of injury or before the visit to the physician will help the athlete’s physician determine the extent of the concussion and when and how the return to play protocol should be initiated.


